‘We’ve never done this before’: How do you vaccinate the world?

The world is rolling out one of the biggest logistical feats in history: vaccinating almost 8 billion people against COVID-19. How is it going? How are politics (and profit) shaping it? And when will life get back to normal?
You are in a queue that could save your life. To combat the worst pandemic the world has seen in a century, scientists have broken records, and governments cut red tape, to deliver vaccines at astonishing speed. But the story isn’t over yet.
Now the shots are here, safe, and more effective than many dared hope, the task of getting them out of the lab and into our arms is coming back to two familiar forces: money and politics.
That’s why in April 2020, the World Health Organisation launched a scheme called COVAX to keep vaccine prices low and dole out doses to countries based on need. It was hoping to avoid the scenes of the last (less deadly) pandemic, swine flu in 2009, when rich nations hoarded vaccine supplies.
But, this time, COVAX is already being undercut by side deals and disputes are again breaking out over exports. Israel has blocked vaccines entering Palestine, for example, and offered to fund others in Syria in exchange for prisoner releases, and a shipment bound for Australia out of Italy has been seized as a new mood of “vaccine nationalism” takes hold in Europe. Meanwhile, China and Russia are jockeying for influence with the West by offering cheaper doses to regions in need through their own brand of “vaccine diplomacy”.
For poorer nations, watching this scramble play out from the end of the vaccine queue can feel a bit like being last to the lifeboats on the Titanic. As West African infectious disease expert Dr Mosoka Fallah says, “Africa is still at the bottom of the boat.”
Now, in an almost Hollywood-style twist of its own, the virus has begun to mutate into variants, some of which may be able to evade vaccine immunity altogether. Scientists warn that nations snapping up more vaccine doses than they need could actually be dragging out the pandemic longer, as the risk of mutants goes up in unprotected populations.
“We can’t keep the virus out, not entirely, so no country is safe until everywhere is safe,” says epidemiologist Professor Michael Toole. “And remember we’ve never done this before. This is the first time in history we’ve tried to vaccinate everyone in the world against a single pathogen.”
So how exactly are we doing it? Who gets which vaccine and when? How much cash are the big pharmaceutical companies making? And when will it all start to make a difference?
Vaccinations in England’s Salisbury Cathedral. The record speed of vaccine development was because of investment not because safety standards were cut.Credit:AP
Which countries are getting the vaccines first?
On December 9, 2020, just a week out from her 91st birthday, the UK’s Margaret Keenan became the first person in the world to receive an approved COVID vaccine. In Australia, the first official shot went to Sydney’s Jane Malysiak, 88, more than two months later, closely followed by Prime Minister Scott Morrison. But many nations are yet to receive a single dose.
So how did Margaret (and the UK) get to the front of the queue?
It comes down not only to early deals done with vaccine makers but where the breakthroughs have happened so far. Governments of countries such as the UK, the US, China and Russia invested in local labs developing vaccines – hence the AstraZeneca vaccine came out of Britain’s Oxford University; the Moderna and the Johnson & Johnson shots were developed in the US; Pfizer in Germany and the US; Sinopharm in China, and Russia named its own home-grown formula Sputnik V after the world-first satellite it put into space in 1957. Other vaccine candidates are likely to be approved as effective too but are further behind in clinical trials, including the Novavax shot developed in the US, of which Australia has already ordered 51 million doses.
There have now been more vaccinations recorded worldwide than COVID cases – more than 390 million doses as of March 18. In Israel, home to the fastest vaccination program, the world has a glimpse of what a post-COVID world might look like. About two-thirds of its 9 million citizens have already received a shot, and half have also had their second dose. The tiny nation of Seychelles is close behind, followed by the United Arab Emirates and then the UK (at about 40 per cent).
The United States is gathering speed at more than 20 per cent, now delivering more than 2 million doses a day. President Joe Biden says there will be enough supply to cover every adult by mid-May. Australia is hoping to pull off the same feat by October, using the Pfizer vaccine for high-priority groups (such as healthcare workers and the elderly) and then AstraZeneca and possibly Novavax for everyone else. But, based on the patchy rollout so far, Australia is unlikely to make that deadline.
India, meanwhile, kicked off the world’s largest vaccination effort in mid-January, aiming to inoculate its first 300 million people by August. (Vaccinating all of India’s 1.4 billion people will likely still take until 2023.) It will rely on the country’s own mammoth election infrastructure to reach people – workers who typically carry voting machines out to remote villages will now haul vaccines on ice.
Women in Mumbai take post-vaccination selfies outside a hospital in March.Credit:Getty Images
These countries are shooting for what is called “herd immunity”, when enough of a population is protected from a virus that it begins to run out of people to infect. The magic number can vary with each disease (and vaccine) but, for COVID, scientists put it somewhere between 70 and 90 per cent of a population. Globally, that’s more than 5 billion people out of the 7.8 billion on Earth.
During the great plagues of the past, people had little choice but to let this immunity build naturally. But vaccines work by teaching your body to mount an immune defence against the virus without you ever having to catch it. What’s injected into your arm will actually disappear from your system quite quickly yet it’s hoped the immunity it triggers will last for some time. All the vaccines approved so far are very effective at stopping severe disease and death from COVID. It is less clear how well they will stop the virus from spreading between people, or hold up against new mutant variants.
Some vaccines appear less effective at stopping milder cases of COVID than the mRNA vaccines by Pfizer and Moderna, which use a new type of technology (about 70 per cent of cases were blocked in trials by AstraZeneca, Johnson & Johnson and Sinopharm versus a 95 per cent efficacy rate for Pfizer and Moderna). But they were all trialed during different surges of the pandemic and scientists stress each of the vaccines approved so far are performing better than expected. Remember, no vaccine at all likely puts your immunity back down to zero.
China, meanwhile, does not appear to be trying to vaccinate its own large population as fast as the West, instead relying on its sweeping surveillance machinery to crush outbreaks fast. Europe’s vaccine rollout has also lagged, hamstrung, some say, by the European Union’s collective vaccine purchase arrangements as well as production delays. Meanwhile, Serbia, outside the EU, is a surprise top performer in the region, benefiting from the vaccine diplomacy push by both Russia and China as they offer cheaper prices for their vaccines than the West. Of course, both countries also leapfrogged the final phase of clinical testing into a “live trial” rollout of sorts, offering assurances via press conference rather than the standard rigorous data.
Russia’s results for Sputnik V, at last peer reviewed and published in leading medical journal The Lancet, have since shown it’s an excellent vaccine, Toole says, with more than 92 per cent efficacy against COVID. “Unfortunately, Putin jumping the gun has created a lot of mistrust, most of all in Russia itself.” Question marks also remain over how Russia can actually deliver on the 2 billion doses it has promised other nations in deals. (On March 9, yet another was signed to produce Sputnik V in Italy, a major step for Russia’s quest to expand the vaccine’s reach into the West. It’s also managed to get around Israel’s block on Sputnik V into Palestine by delivering doses through Egypt with help from the UAE.)
As for China’s vaccines, the data is less clear, limited to the results published by other countries running trials, such as the UAE. But Toole says they too look quite effective.
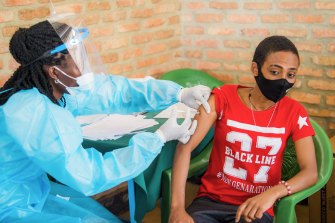
In Rwanda, a young man receives his first dose of vaccine in March.Credit:Getty Images
Why aren’t vaccines being rolled out equally?
Manufacturers are promising to deliver about 5 billion vaccine doses between them by the end of 2021. Considering all of the vaccines (save the very latest approved from Johnson & Johnson) require two doses, that’s enough for less than 3 billion people. And more than half of this supply is already tied up in deals with rich nations. Canada has ordered more than five times what it needs to vaccinate its people, Australia almost four times as much, and the UK and US are also well in excess.
At this rate, researchers estimate at least a two-year gap between when wealthy nations roll out most of their vaccines and the rest of the world can. The WHO-led allocation model, COVAX, has deals in place for 2 billion vaccine doses so far, and wants to distribute 1.3 billion of these under subsidy to low-income countries by the end of 2021. While high-income countries can buy enough from the COVAX pot to cover up to 50 per cent of their populations, the idea is for everyone to get vaccines for their most vulnerable 20 per cent (such as frontline workers) first.
At Médecins Sans Frontières, Kate Elder says the model is well-intentioned but too slow. As of March, it was well behind schedule, having struggled to secure funds from its member countries, though hundreds have signed on, including Australia, and now the US with a late but welcome $4 billion cash injection.
The first free shipment of COVAX vaccines touched down in Ghana only in late February. Africa is expected to get only enough doses to vaccinate 3 per cent of the population by mid-2021.
Toole says rich countries don’t just need to up their financial contributions to COVAX; they need to step back and allow it room in the market to buy the vaccines needed, instead of making their own deals.
Australian COVID adviser to the WHO, Professor Mary-Louise McLaws, agrees. “Had everyone just relied on COVAX it might have worked well,” she says. “But it’s difficult because, of course, countries want to protect their citizens first.”
Africa, Fallah says, tried to do its part and keep the virus out – governments shut airports and even imposed lockdowns at great economic cost. Now their existing debts are worse. They can’t buy vaccines at current prices. They need COVAX.
“It can’t fail,” he says. “It has to be accelerated.”
Of course, if you were doling out doses blindly based on outbreaks, much of your focus would actually be on the West. The developing world typically bears the brunt of infectious diseases (think malaria and Ebola) but so far most of COVID’s big waves have hit wealthier nations harder, from the US to Europe.
Part of the reason why Western countries ordered excess doses is that no one knew exactly which lab would get their vaccine over the line. Australia’s own attempt at a home-grown vaccine using new “molecular clamp” technology, for example, was called off in late 2020, and the Australian government’s order of 50 million doses scrapped.
Much of the world’s excess stock is now expected to be donated or sold on. New Zealand, which has reserved about three times as much as it needs, has already committed to giving some to its neighbouring Pacific Islands. Canada looks likely to donate too. And Australia has joined forces with other countries in its Indo-Pacific alliance the Quad – the US, India, and Japan – to roll out a new vaccine diplomacy campaign aimed at countering Chinese influence in the region by delivering 1 billion doses by the end of 2022. (Australia is also sending 8000 urgent doses to Papua New Guinea as the nearby nation grapples with a fast-growing outbreak.)
But Toole and McLaws say there must be a binding commitment from countries to pass on their excess doses – fast – to countries in need and at low or zero cost.
“This is no longer just an issue of morality but global security,” Fallah says.
Israel has begun vaccinating some Palestinians working in Israel after copping criticism for blocking doses into the West Bank. Credit:Getty
So when will vaccines end the pandemic? And what about variants?
As lockdowns and increased immunity slow down the virus, its evolution is speeding up – and mutations in its genetic code that allow it to spread faster or better infect new hosts are rapidly taking over. “This is life or death for the virus now,” Toole says. “It’s trying to survive.”
Most of the UK’s cases are now caused by a variant known as B117, not just more contagious but considered more deadly too. In South Africa, another more transmissible variant has arisen that shows signs of at least partially evading vaccine immunity. And in Manaus, Brazil, the first city in the world thought to have reached herd immunity has been hit by an even worse second wave. The culprit? Another mutant lineage of the virus able to reinfect both COVID survivors and those vaccinated.
While vaccines will play a big role in ending the pandemic, governments must plan for COVID to be with us for some time yet, possibly, Toole says, as a seasonal illness requiring a new booster shot each year to fight off variants (in the same way we inoculate against the fast-evolving flu).
Scientists are holding their breath as they watch Europe, the US and the UK, countries with both lots of virus and large-scale vaccine rollouts. “If you are vaccinated in the early days of [having caught the virus], you can become a kind of living test tube for the variant to get around the vaccine,” McLaws says. “It’s going to be a horror show if these become playgrounds for the virus to mutate again.”
US infectious disease expert Michael Osterholm has likened the emerging variants to a hurricane on the horizon, bearing down on the relative calm in the middle of the pandemic. He fears the UK variant, which is already doubling in the US the way it did in Europe, will trigger another out-of-control wave in his country and wants first-dose vaccinations to be prioritised over second shots, as has been done in the UK and now Canada. This will mean more people have at least some immunity, even if it’s not as strong. But McLaws warns that lockdowns in the UK may be masking the true effect of such an experiment.
In California, people stand in a church carpark to wait for vaccines from a pop-up clinic in March. Credit:Getty Images
Experts say vaccines, even those deemed less effective against variants, will likely still cover people from the most severe cases of COVID. Still, Toole says that alone is not enough. “As long as the virus keeps circulating, there can be more variants.”
Vaccine companies are now considering how best to roll out tweaked formulas to cover variants, which many regulators have already promised to fast-track. Australia’s COVID-19 vaccine maker CSL says it’s open to making such an AstraZeneca booster but has warned they wouldn’t be available until at least the end of 2021.
Toole says the Pfizer and Moderna mRNA vaccine technology is the fastest to tweak (but the most expensive to roll out given they need to be kept frozen). Meanwhile, Oxford University is considering how people might respond to combinations of different vaccines in case other types are needed for boosters.
Fallah worries when boosters will arrive for the developing world given the delay so far. “We will get the vaccine very late and it may not work.”
While South Africa cancelled its order of AstraZeneca after the vaccine’s disappointing results against the variant in circulation there, Johnson & Johnson’s has shown more promise (57 per cent efficacy overall and 85 per cent for preventing severe disease). Given this is also a single shot with less expensive storage requirements than the mRNA vaccines, Toole and McLaws say it could be a game-changer for the developing world.
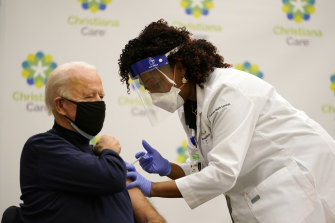
US President Joe Biden received his first dose of the Pfizer vaccine in December on live TV.Credit: AP
Do we need to rein in vaccine companies profiting from the pandemic?
In the early days of the pandemic, before any vaccine had been approved, the chief executive of the world’s biggest vaccine maker took a gamble. Adar Poonawalla runs the Serum Institute in India, and began investing millions of his own dollars into scaling up production for a rapid COVID rollout, from stockpiling glass vials to building new facilities. The company is now helping supply India, and in agreements with COVAX and dozens more nations for COVID shots, having reached a deal with AstraZeneca to make a generic copy of its vaccine called COVIDShield.
This may seem like an obvious solution – if the companies behind the vaccines cannot make doses fast enough to meet demand, why not call off intellectual property (IP) rights until the global crisis is over? The inventor of the polio vaccine, Jonas Salk, famously didn’t patent it.
But when India, Africa and other nations took this idea to the World Trade Forum, a group of wealthy countries, including the US and Australia, blocked it. They argue suspending IP, even just for the length of the pandemic, could stifle innovation and discourage companies from sharing breakthroughs. (The EU also opposed the move but is now threatening to strip AstraZeneca of its IP after it missed production deadlines.)
So far AstraZeneca has allowed others to produce its vaccine – not just in India but in Australia and South Korea. Johnson & Johnson will license its vaccine in South Africa and Novavax in India. Johnson & Johnson and AstraZeneca have also pledged to sell their vaccines at cost (covering only the price of production), though experts point out that company deals across the board remain shrouded in secrecy. And, in some cases, manufacturers are charging prices found to be “among the highest of any in existence for vaccines”.
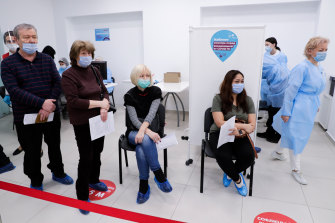
In Moscow, people line up for a Sputnik jab, which they don’t have to make an appointment for at this shopping plaza pop-up. Credit:Getty Images
While companies still need to make a living, Elder and other experts argue that a record amount of public money went into their vaccines (an estimated $10 billion collectively in public and not-for-profit funding) and therefore governments should crack down on high prices and monopolies.
Fallah says that, during a pandemic, there must be a ceiling to profits. “Do we really want to create more billionaires or do we want to get the world back to normal?”
McLaws agrees there should be a global rule to UN membership that curbs profit and blocks IP until the storm has passed. “There has to be a way to find a balance [without discouraging development]. We are all at risk of dying.”
Fallah points to the example of HIV antivirals. When the IP was scrapped, prices went down, allowing the desperately needed drugs to better reach Africa. To fight Ebola, the world has a stockpile managed by charities that can be drawn on whenever there is an outbreak. “Sometimes you can get them within two hours,” says Fallah, who has helped on many Ebola vaccination campaigns.
Slovak Prime Minister Igor Matovic, right, and Health Minister Marek Krajci oversee the arrival of a shipment of the Russian vaccine Sputnik V into Slovakia.Credit:AP
How do you actually get vaccines to everyone anyway?
Toole himself has run vaccination campaigns in some of the most remote and dangerous parts of the world, from Malawi to Northern Iraq, where he recalls training US special forces to deliver injections. “It’s difficult but we already have volunteers on the ground in these areas ready to go,” he says. “Of course, they won’t be using the mRNA vaccines, Pfizer [and Moderna]. They’re too costly [to roll out].”
Given the scale of the task ahead, new technology and infrastructure is needed for even the more standard vaccines. QR codes are helping track batches around the world. In Israel, a text message will tell you when it’s your turn for a shot. In Italy, vaccination kiosks are popping up in the street, decorated with purple flowers. Elsewhere, cathedrals, school halls and stadiums play host to mass inoculations.
McLaws says the work under way now will allow for faster responses for upcoming booster shots – and future pandemics. But she notes almost all countries ignored warnings in early 2020 to plan for the rollout. “Even in Australia, where we’ve been at times remarkable on [COVID]. We didn’t go to GPs and pharmacies straight away, we didn’t start training for multi-dose vaccines.”
If the void in vaccine supply remains open for the developing world, Fallah warns the black market will fill it with fakes. Already large shipments of knockoffs have been seized in China and South Africa. ”We have to move fast before people lose confidence,” he says.
Vaccine hesitancy is also a problem in high-income countries (and Russia has already been accused by US intelligence agencies of spreading misinformation about rival Western vaccines).But McLaws is more concerned about rollout oversights missing low socioeconomic groups altogether. She warns there could also be a tale of two vaccination programs in the West – one for those on higher incomes, already well connected with their health services, while the most vulnerable fall through the cracks.
Even under Israel’s proactive rollout strategy, many in the lowest socioeconomic groups are being missed. McLaws says most programs, including Australia’s, look likely to make the same mistake. On March 18, a federal government spokeswoman said the Commonwealth began planning for the rollout in June 2020 with the creation of a vaccine taskforce but was still working with states and community groups to “identify the most appropriate methods to reach vulnerable populations, including the homeless and people in social housing to ensure these hard to reach groups have access to COVID-19 vaccination”.
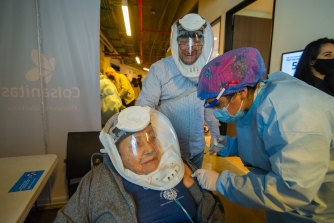
In Bogota in Colombia, the first shot of China’s Sinovac is given to a woman aged over 80.Credit:Getty Images
What happens next?
Once vaccination programs are further under way, most experts envision a “vaccine passport” model will allow more international travel, similar to the yellow fever papers once widely required of travellers. But McLaws and Toole warn a vaccine is never an absolute guarantee against infection, especially for a fast-evolving virus such as COVID.
“When you’re outside Australia, you may still need to wear a mask and distance for some time,” McLaws says.
The task of vaccinating the world is likely to take longer than hoped, but Fallah knows that the market forces now delaying equal access to vaccines also underpin the case to speed it up. After all, the more parts of the world that are vaccinated, the better it will be for everyone’s bottom line.
“If they don’t help the rest of us, they’ll have to spend more anyway to create new vaccines,” he says.
“The world came together and eliminated smallpox … We are one people, we are travellers. This is for everyone.”
If you'd like some expert background on an issue or a news event, drop us a line at [email protected] or [email protected]. Read more explainers here.
Most Viewed in National
Source: Read Full Article