How a jogging accident saved Andrew’s life – from lung cancer

Save articles for later
Add articles to your saved list and come back to them any time.
When Gavin Wright became a surgeon 22 years ago, it was unusual for him to encounter lung cancer patients who had never smoked.
These days, the research and education lead at the Victorian Comprehensive Cancer Centre estimates that about 20 per cent of the lung cancer patients he operates on have no substantial smoking history.
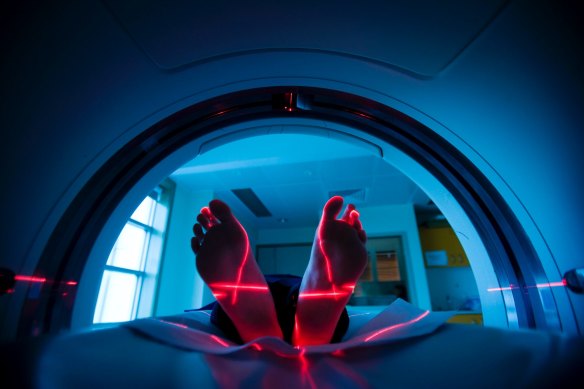
While the incidence of lung cancer has dropped in Australia due to a decline in tobacco smoking, the Victorian Lung Cancer Registry says an increasing number of non-smokers are now being diagnosed.Credit: Nicolas Walker
“It’s gone from rare to not uncommon,” the associate professor said.
Wright believes that pollution is driving the increase in lung cancer among non-smokers, with women and people from Asian backgrounds at heightened risk.
Almost 30 per cent of Australian women diagnosed with lung cancer have never smoked, compared with 16 per cent of men, according to the most recent figures from cancer research centre the Daffodil Centre.
While the incidence of lung cancer has dropped in Australia due to a decline in tobacco smoking, “an increasing number of non-smokers (mainly women) are now being diagnosed with lung cancer”, according to a 2022 report from the Victorian Lung Cancer Registry, which is managed by Monash University.
Andrew Ure was diagnosed with lung cancer in 2020 after he tripped over a tree root and broke his arm while jogging at dusk along the Yarra River.
Doctors at the Epworth in Richmond ordered a precautionary scan of his chest because they were worried he may have injured his lungs during the fall.
“The radiologist said, ‘There is something on your right lung, when you get through all of this, you might want to get it checked out’,” Ure said.
Ure initially decided to monitor the small shadow on his lung with scans every three months, but after more than a year his surgeon told him it had grown 20 per cent and should be removed.
Andrew Ure was diagnosed with lung cancer in 2020.Credit: Joe Armao
Testing confirmed it was cancer.
“When the word ‘cancer’ came up I was shocked,” the 52-year-old engineer said.
“I didn’t think I was at risk because I had never smoked. Not even a puff.”
Ure wonders whether his cancer was linked to the 16 years he worked as an engineer in Thailand, where air quality is poor. His surgeon told him this was unlikely as his cancer was located in one spot, rather than throughout his lung.
“I was fortunate it was picked up so early,” said Ure, who has been in remission for more than a year.
“Through an unlucky accident I detected something that could’ve been life-threatening.”
The rise in non-smokers developing lung cancer is playing out across the world and was discussed at the Radiological Society of North America’s annual meeting in Chicago last month.
Dr Atul Gupta, Philips’ chief medical officer of image-guided therapy, said the company had rolled out mobile CT scanners in New York State in the US and in Australia to ensure at-risk groups were screened for lung cancer, including those who had never smoked.
“It’s a way of increasing access to care,” he said.
Heart of Australia operates mobile trucks fitted out with diagnostic medical equipment
Heart of Australia, the mobile healthcare company that Philips has partnered with in Australia, has five trucks fitted out with medical diagnostic equipment, including one that contains the world’s first battery-powered CT scanner that screens the lungs of current and former miners in Queensland.
Heart of Australia head of operations Ewan Wylie said their clinicians were detecting lung cancer and disease – such as silicosis, emphysema and chronic bronchitis – in about one in seven retired miners.
“They often worked in very heavy dust,” he said.
Australians aged 50 to 70 years who have a history of heavy cigarette smoking will receive low-dose CT scans every two years under a $264 million federal government program that will be rolled out from July 2025.
To qualify, they must have smoked a packet of cigarettes a day for 30 years.
Wylie is concerned the scheme won’t capture thousands of Australians at heightened risk of lung cancer due to workplace exposure to silica dust, asbestos and diesel emissions.
Lung Foundation Australia chief executive Mark Brooke believes the initiative strikes the right balance between being affordable and targeting those most at risk.
He said it was important to avoid stigmatising smokers who had been diagnosed with lung cancer.
“They are unfairly blamed,” he said. “This is an addiction like any other addiction.”
Lung cancer is the leading cause of cancer deaths in Australia and has one of the lowest five-year survival rates at 24 per cent.
“For the majority of Australians, diagnosis is too late… it’s usually picked up in stage three and four,” Brooke said.
“This screening program will enable us to detect lung cancer much earlier when we’ve got much greater opportunity to prolong life through treatment.”
The author travelled to the US courtesy of Philips.
Get the day’s breaking news, entertainment ideas and a long read to enjoy. Sign up to receive our Evening Edition newsletter.
Most Viewed in National
From our partners
Source: Read Full Article